Health Library
Breast Eczema: Causes, Symptoms, and How to Manage It
February 19, 2026
Question on this topic? Get an instant answer from August.
Breast eczema is a form of eczema (atopic dermatitis) that causes dry, itchy, and inflamed skin on or around the breasts. It can show up on the nipples, areola (darker circle around nipple), under breasts, between breasts, or on chest. It is not contagious, and it is more common than you might think.
If your breast skin feels irritated, flaky, or sore.

What Does Breast Eczema Look Like?
Breast eczema looks a lot like eczema anywhere else on body. The skin becomes red or discolored, dry, and scaly. You may notice small bumps, flaking, or rough patches.
In some cases, skin may crack, ooze clear fluid, or form a crust. This tends to happen during more severe flare ups. The area often feels intensely itchy, and scratching can make irritation worse.
On nipples and areola, eczema may cause peeling, cracking, or a burning sensation. The skin in this area is especially thin and sensitive, so flare ups here can be particularly uncomfortable. A systematic review published in PubMed noted that nipple eczema can present as atopic, irritant, or allergic contact eczema, and it often reduces quality of life for those affected.
Breast eczema can affect one or both breasts. The area under breasts also common, especially where skin folds trap moisture and heat.
What Causes Breast Eczema?
Eczema happens when skin barrier (outer protective layer of your skin) does not function properly. This barrier normally locks in moisture and keeps out irritants. When it breaks down, skin becomes dry, sensitive, and prone to inflammation.
Several factors can contribute to breast eczema. Here are most common ones.
- Genetics play a big role. If you have a family history of eczema, asthma, or hay fever, you are more likely to develop it. Research published in NCBI StatPearls database explains that mutations in filaggrin gene (FLG) can weaken skin barrier and make eczema more likely.
- Irritants like harsh soaps, laundry detergents, perfumes, and certain fabrics (especially wool and synthetic materials) can trigger flare ups on breast area.
- Allergens can also cause or worsen eczema. Contact allergens like nickel (from bra underwires or piercings), lanolin, fragrances, and even some topical creams can lead to allergic contact dermatitis on breasts.
- Sweat and moisture buildup, particularly under breasts or inside a tight fitting bra, can irritate skin and trigger a flare.
- Hormonal changes during menstruation, pregnancy, or breastfeeding can affect skin and increase sensitivity.
- Stress is a well known trigger. Emotional stress can cause or worsen eczema flare ups by affecting immune system's response.
Understanding what triggers your flare ups one of most helpful steps you can take. It may take some trial and error, but identifying your specific triggers gives you more control.
Can Breastfeeding Cause or Worsen Breast Eczema?
Yes, breastfeeding can trigger or aggravate eczema on nipples and areola. The constant friction from latching, along with exposure to saliva and moisture, can irritate already sensitive skin.
A case report published in PMC described a woman with severe nipple eczema since puberty who received guided care during pregnancy and postpartum. With right combination of topical treatment, breastfeeding guidance, and emotional support, she was able to breastfeed successfully.
If you are breastfeeding and notice cracking, redness, or soreness around nipples, talk to your doctor. Topical corticosteroids and calcineurin inhibitors are considered safe during breastfeeding when used correctly. Apply them right after nursing and gently wipe area before next feeding.
How Is Breast Eczema Diagnosed?
In most cases, a healthcare provider can diagnose breast eczema just by looking at skin. They will examine affected area and ask about your symptoms, triggers, and medical history.
If diagnosis is unclear, your doctor may order additional tests. These can include allergy testing to check for specific contact allergens, a skin biopsy to rule out other conditions, or blood work to look for signs of infection.
There is one important condition to be aware of. Paget's disease of breast a rare form of breast cancer that can mimic appearance of nipple eczema. It causes redness, crusting, and itching on nipple. However, there are some differences. Paget's disease usually affects only one nipple, while eczema tends to affect both. Paget's disease also does not respond to eczema treatments. If your symptoms persist despite treatment, your doctor may recommend a mammogram or biopsy to rule it out.
What Are Treatment Options?
There is no cure for eczema, but right approach can keep symptoms under control and reduce flare ups.
The first step is daily skin care. Moisturize breast area at least twice a day with a fragrance free emollient or ointment. The thicker moisturizer, better it seals in moisture. Apply it within a few minutes of bathing to lock in hydration.
For active flare ups, your doctor may recommend a topical corticosteroid. Mild to moderate strength steroids work well for most cases. They reduce inflammation and calm itching quickly. For sensitive areas like nipples, a topical calcineurin inhibitor (like tacrolimus or pimecrolimus) may be preferred because it does not thin skin with long term use.
If eczema becomes infected from scratching, your doctor may prescribe a short course of antibiotics. People with eczema are more prone to bacterial skin infections, especially with Staphylococcus.
For more stubborn cases, your doctor might explore newer options like dupilumab, a biologic medication that targets specific immune pathways involved in eczema.
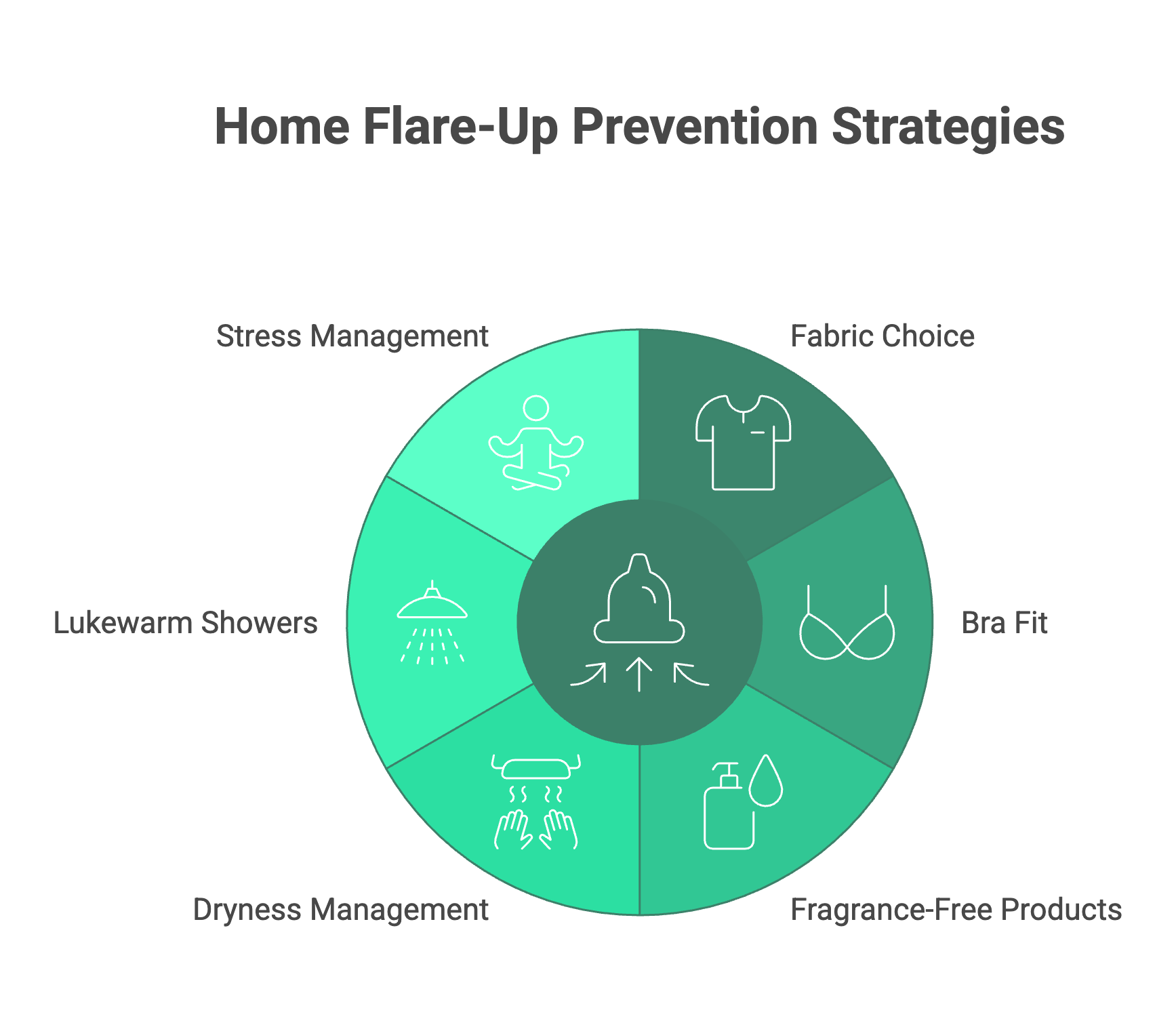
What Can You Do at Home to Prevent Flare Ups?
Preventing flare ups is just as important as treating them. Small changes in your daily routine can make a big difference.
- Wear soft, breathable fabrics like cotton. Avoid wool and rough synthetics that rub against skin.
- Choose a well fitting bra that does not squeeze or trap moisture. Bras with smooth seams and no underwire may be gentler on sensitive skin.
- Use fragrance free soaps, lotions, and laundry detergents. Even products labeled "gentle" can contain irritants.
- Keep area under breasts dry. Pat skin gently after bathing and consider using a thin cotton liner to absorb moisture.
- Take lukewarm showers instead of hot ones. Hot water strips moisture from skin and can trigger itching.
- Manage stress through activities that work for you, whether that is walking, deep breathing, or talking with someone you trust.
If you are dealing with itchy, inflamed skin and wondering whether it could be a different type of eczema, this on papular eczema may give you more clarity.
Can Breast Eczema Be Confused with Other Conditions?
Yes. Several skin conditions can look similar to breast eczema, so getting right diagnosis matters.
Fungal infections (like candidiasis) under breast can cause redness and itching, but they usually come with a distinct border and sometimes a yeasty smell. Psoriasis can also cause scaly patches, but scales tend to be thicker and more silvery.
Contact dermatitis from a specific product or material may look identical to eczema. The key difference is that contact dermatitis improves once trigger is removed.
And as mentioned, Paget's disease rare but serious condition that should always be ruled out if nipple changes do not respond to standard eczema treatment.
Eczema can sometimes look like other conditions, including ringworm. If you notice coin shaped patches, this comparison of nummular eczema versus ringworm can help you tell them apart.
Bottom Line
Breast eczema is a common, manageable condition. It can cause real discomfort, but with the right skin care routine, trigger avoidance, and treatment plan, most people see significant improvement. If your symptoms do not respond to basic care or if you notice changes on only one nipple, see your doctor to rule out other conditions. You deserve skin that feels comfortable, and there are effective ways to get there.
Health Companion
trusted by
6Mpeople
Get clear medical guidance
on symptoms, medications, and lab reports.